Abstract
Background
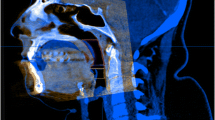
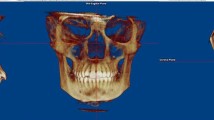
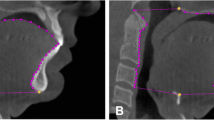
A reliable method for analyzing the upper airway (UA) remains a challenge. This study aimed to report the methods for UA assessment using cone-beam computed tomography (CBCT) in adults with obstructive sleep apnea (OSA).
Methods
We performed a systematic review (PROSPERO #CRD42021237490 and PRISMA checklist) that applied a search strategy to seven databases and grey literature.
Results
In 29 studies with moderate-to-high risk of bias, investigators mostly reported the body position during CBCT (upright or supine) and hard tissue references, diverging in UA delimitation and terminologies. The meta-analysis showed two subgroups (upright and supine), and no statistical differences were identified (p = 0.18) considering the UA area. The volume in the OSA group was smaller than that in the control group (p < 0.003 and Cohen’s d = − 0.81) in the upright position. Patients with OSA showed smaller anteroposterior dimensions than the control group and were not affected by the position during image acquisition (p = 0.02; Cohen’s d = − 0.52). The lateral measurements were also lower in the OSA group (supine) (p = 0.002; Cohen’s d = − 0.6).
Conclusions
Patients with OSA showed smaller UA measurements in the upright (volume) and supine (lateral dimension) positions. The anteroposterior dimension was also reduced in patients with OSA compared to the control group, regardless of the position during CBCT acquisition.








Similar content being viewed by others
References
Benjafield AV, Ayas NT, Eastwood PR, Heinzer R, Ip MSM, Morrell MJ, Nunez CM, Patel SR, Penzel T, Pépin JL, Peppard PE, Sinha S, Tufik S, Valentine K, Malhotra A (2019) Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Respir Med 7(8):687–698. https://doi.org/10.1016/S2213-2600(19)30198-5
Fabbro CD, Chaves CM Jr, Bittencourt LRA, Tufik S (2010) Clinical and polysonographic assessment of the BRD Appliance in the treatment of obstructive sleep apnea syndrome. Dental Press J Orthod 15(1):107–117
Neelapu BC, Kharbanda OP, Sardana HK, Balachandran R, Sardana V, Kapoor P, Gupta A, Vasamsetti S (2017) Craniofacial and upper airway morphology in adult obstructive sleep apnea patients: a systematic review and meta-analysis of cephalometric studies. Sleep Med Rev 31:79–90. https://doi.org/10.1016/j.smrv.2016.01.007
Kapur VK, Auckley DH, Chowdhuri S, Kuhlmann DC, Mehra R, Ramar K, Harrod CG (2017) Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: an american academy of sleep medicine clinical practice guideline. J Clin Sleep Med 13(3):479–504. https://doi.org/10.5664/jcsm.6506
Boulos MI, Jairam T, Kendzerska T, Im J, Mekhael A, Murray BJ (2019) Normal polysomnography parameters in healthy adults: a systematic review and meta-analysis. Lancet Respir Med 7(6):533–543. https://doi.org/10.1016/S2213-2600(19)30057-8
Brown AA, Scarfe WC, Scheetz JP, Silveira AM, Farman AG (2009) Linear accuracy of cone beam CT derived 3D images. Angle Orthod 79(1):150–157. https://doi.org/10.2319/122407-599.1
Cheng S, Brown EC, Hatt A, Butler JE, Gandevia SC, Bilston LE (2014) Healthy humans with a narrow upper airway maintain patency during quiet breathing by dilating the airway during inspiration. J Physiol 592(21):4763–4774. https://doi.org/10.1113/jphysiol.2014.279240
Zhao Y, Raco J, Kourmatzis A, Diasinos S, Chan HK, Yang R, Cheng S (2020) The effects of upper airway tissue motion on airflow dynamics. J Biomech 99:109506. https://doi.org/10.1016/j.jbiomech.2019.109506
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Moher D (2021) Updating guidance for reporting systematic reviews: development of the PRISMA 2020 statement. J Clin Epidemiol 134:103–112. https://doi.org/10.1016/j.jclinepi.2021.02.003
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A (2016) Rayyan-a web and mobile app for systematic reviews. Syst Rev 5(1):210. https://doi.org/10.1186/s13643-016-0384-4
Bruwier A, Poirrier R, Albert A, Maes N, Limme M, Charavet C, Milicevic M, Raskin S, Poirrier AL (2016) Three-dimensional analysis of craniofacial bones and soft tissues in obstructive sleep apnea using cone beam computed tomography. Int Orthod 14(4):449–461. https://doi.org/10.1016/j.ortho.2016.10.003
Ogawa T, Enciso R, Shintaku WH, Clark GT (2007) Evaluation of cross-section airway configuration of obstructive sleep apnea. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 103(1):102–108. https://doi.org/10.1016/j.tripleo.2006.06.008
Wang SH, Keenan BT, Wiemken A, Zang Y, Staley B, Sarwer DB, Torigian DA, Williams N, Pack AI, Schwab RJ (2020) Effect of weight loss on upper airway anatomy and the apnea-hypopnea index. The importance of tongue fat. Am J Respir Crit Care Med 201(6):718–727l. https://doi.org/10.1164/rccm.201903-0692OC
Senaratna CV, Perret JL, Lodge CJ, Lowe AJ, Campbell BE, Matheson MC, Hamilton GS, Dharmage SC (2017) Prevalence of obstructive sleep apnea in the general population: a systematic review. Sleep Med Rev 34:70–81. https://doi.org/10.1016/j.smrv.2016.07.002
Andrade C (2020) Sample Size and its Importance in Research. Indian J Psychol Med 42(1):102–103. https://doi.org/10.4103/IJPSYM.IJPSYM_504_19
Souza FJ, Evangelista AR, Silva JV, Périco GV, Madeira K (2016) Cervical computed tomography in patients with obstructive sleep apnea: influence of head elevation on the assessment of upper airway volume. J Bras Pneumol 42(1):55–60. https://doi.org/10.1590/S1806-37562016000000092
Hsu WE, Wu TY (2019) Comparison of upper airway measurement by lateral cephalogram in upright position and CBCT in supine position. J Dent Sci 14(2):185–191. https://doi.org/10.1016/j.jds.2019.01.007
Kamaruddin N, Daud F, Yusof A, Aziz ME, Rajion ZA (2019) Comparison of automatic airway analysis function of Invivo5 and Romexis software. PeerJ 7:e6319. https://doi.org/10.7717/peerj.6319.eCollection2019
Chen H, van Eijnatten M, Wolff J, de Lange J, van der Stelt PF, Lobbezoo F, Aarab G (2017) Reliability and accuracy of three imaging software packages used for 3D analysis of the upper airway on cone beam computed tomography images. Dentomaxillofac Radiol 46(6):20170043. https://doi.org/10.1259/dmfr.20170043
Gomes AF, Brasil DM, Silva AIV, Freitas DQ, Haiter-Neto F, Groppo FC (2020) Accuracy of ITK-SNAP software for 3D analysis of a non-regular topography structure. Oral Radiol 36(2):183–189. https://doi.org/10.1007/s11282-019-00397-y
Pinheiro ML, Yatabe M, Ioshida M, Orlandi L, Dumast P, Trindade-Suedam IK (2018) Volumetric reconstruction and determination of minimum crosssectional area of the pharynx in patients with cleft lip and palate: comparison between two different softwares. J Appl Oral Sci 26:e20170282. https://doi.org/10.1590/1678-7757-2017-0282
Ruellas ACDO, Tonello C, Gomes LR, Yatabe MS, Macron L, Lopinto J, Goncalves JR, Garib Carreira DG, Alonso N, Souki BQ, Coqueiro Rda S, Cevidanes LH (2016) Common 3-dimensional coordinate system for assessment of directional changes. Am J Orthod Dentofacial Orthop 149(5):645–656. https://doi.org/10.1016/j.ajodo.2015.10.021
Brown EC, Cheng S, McKenzie DK, Butler JE, Gandevia SC, Bilston LE (2015) Tongue stiffness is lower in patients with obstructive sleep apnea during wakefulness compared with matched control subjects. Sleep 38(4):537–544. https://doi.org/10.5665/sleep.4566
Ball M, Hossain M, Padalia D (2021) Anatomy, Airway. StatPearls. Statpearls Publishing Copyright © 2021, StatPearls Publishing LLC, Treasure Island
Rodrigues MM, Pereira Filho VA, Gabrielli MFR, Oliveira TFMD, Batatinha JAP, Passeri LA (2017) Volumetric evaluation of pharyngeal segments in obstructive sleep apnea patients. Braz J Otorhinolaryngol S1808–8694(17):30001. https://doi.org/10.1016/j.bjorl.2016.12.001
Hong QN, Pluye P, Fàbregues S, Bartlett G, Boardman F, Cargo M, Dagenais P, Gagnon MP, Griffiths F, Nicolau B, O’Cathain A, Rousseau MC, Vedel I (2019) Improving the content validity of the mixed methods appraisal tool: a modified e-Delphi study. J Clin Epidemiol 111:49-59.e41. https://doi.org/10.1016/j.jclinepi.2019.03.008
Shigeta Y, Enciso R, Ogawa T, Shintaku WH, Clark GT (2008) Correlation between retroglossal airway size and body mass index in OSA and non-OSA patients using cone beam CT imaging. Sleep Breath 12(4):347–352. https://doi.org/10.1007/s11325-008-0186-6
Haskell JA, McCrillis J, Haskell BS, Scheetz JP, Scarfe WC, Farman AG (2009) Effects of mandibular advancement device (MAD) on airway dimensions assessed with cone-beam computed tomography. Semin Orthod 15(2):132–158. https://doi.org/10.1053/j.sodo.2009.02.001
Enciso R, Nguyen M, Shigeta Y, Ogawa T, Clark GT (2010) Comparison of cone-beam CT parameters and sleep questionnaires in sleep apnea patients and control subjects. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 109(2):285–293. https://doi.org/10.1016/j.tripleo.2009.09.033
Abi-Ramia LBP, Carvalho FAR, Coscarelli CT, Almeida MAdO (2010) Aparelho de avanço mandibular aumenta o volume da via aérea superior de pacientes com apneia do sono. Dental Press J Orthod 15(5):166–171. https://doi.org/10.1590/S2176-94512010000500020
Enciso R, Shigeta Y, Nguyen M, Clark GT (2012) Comparison of cone-beam computed tomography incidental findings between patients with moderate/severe obstructive sleep apnea and mild obstructive sleep apnea/healthy patients. Oral Surg Oral Med Oral Pathol Oral Radiol 114(3):373–381. https://doi.org/10.1016/j.oooo.2012.03.014
Schendel SA, Broujerdi JA, Jacobson RL (2014) Three-dimensional upper-airway changes with maxillomandibular advancement for obstructive sleep apnea treatment. Am J Orthod Dentofacial Orthop 146(3):385–393. https://doi.org/10.1016/j.ajodo.2014.01.026
Butterfield KJ, Marks PLG, McLean L, Newton J (2015) Pharyngeal airway morphology in healthy individuals and in obstructive sleep apnea patients treated with maxillomandibular advancement: a comparative study. Oral Surg Oral Med Oral Pathol Oral Radiol 119(3):285–292. https://doi.org/10.1016/j.oooo.2014.11.016
Butterfield KJ, Marks PLG, McLean L, Newton J (2015) Linear and volumetric airway changes after maxillomandibular advancement for obstructive sleep apnea. J Oral Maxillofac Surg 73(6):1133–1142. https://doi.org/10.1016/j.joms.2014.11.020
Cossellu G, Biagi R, Sarcina M, Mortellaro C, Farronato G (2015) Three-dimensional evaluation of upper airway in patients with obstructive sleep apnea syndrome during oral appliance therapy. J Craniofac Surg 26(3):745–748. https://doi.org/10.1097/SCS.0000000000001538
Van Leeuwen M, Martinez-Ferrate R, Preble D, Hanewinkel W, Gleeson M, Andra J (2015) A two-dimensional gauge and protocol for fitting oral appliances used in treating sleep breathing disorders. Compend Contin Educ Dent 36(2):140-142-144–145
Buchanan A, Cohen R, Looney S, Kalathingal S, De Rossi S (2016) Cone-beam CT analysis of patients with obstructive sleep apnea compared to normal controls. Imag Sci Dent 46:9–16. https://doi.org/10.5624/isd.2016.46.1.9
Chaves Junior CM, Maciel SSC, Gurgel ML, Silva PGB, Ribeiro TR, Kurita LM (2016) Efeitos do aparelho reposicionador mandibular no tratamento da apneia obstrutiva do sono. Ortho Sci: Orthod Sci Pract 9:36–45
Tikku T, Khanna R, Sachan K, Agarwal A, Srivastava K, Lal A (2016) Dimensional and volumetric analysis of the oropharyngeal region in obstructive sleep apnea patients: a cone beam computed tomography study. Dent Res J (Isfahan) 13(5):396–404. https://doi.org/10.4103/1735-3327.192273
Shete CS, Bhad WA (2017) Three-dimensional upper airway changes with mandibular advancement device in patients with obstructive sleep apnea. Am J Orthod Dentofac Orthop 151(5):941–948. https://doi.org/10.1016/j.ajodo.2016.09.025
Chen H, Li YG, Reiber JHC, de Lange J, Tu S, van der Stelt P, Lobbezoo F, Aarab G (2018) Analyses of aerodynamic characteristics of the oropharynx applying CBCT: obstructive sleep apnea patients versus control subjects. Dentomaxillofac Radiol 47(2):20170238. https://doi.org/10.1259/dmfr.20170238
Veys B, Pottel L, Mollemans W, Abeloos J, Swennen G, Neyt N (2017) Three-dimensional volumetric changes in the upper airway after maxillomandibular advancement in obstructive sleep apnoea patients and the impact on quality of life. Int J Oral Maxillofac Surg 46(12):1525–1532. https://doi.org/10.1016/j.ijom.2017.06.020
Momany SM, AlJamal G, Shugaa-Addin B, Khader YS (2018) Cone Beam computed tomography analysis of upper airway measurements in patients with obstructive sleep apnea. Am J Med Sci 352(4):376–384. https://doi.org/10.1016/j.amjms.2016.07.014
Frey R, Gabrielova B, Gladilin E (2018) A combined planning approach for improved functional and esthetic outcome of bimaxillary rotation advancement for treatment of obstructive sleep apnea using 3D biomechanical modeling. PLoS ONE 13(8):e0199956. https://doi.org/10.1371/journal.pone.0199956
Molaei S, Esmaeili F, Sadrhaghighi A, Khatoonabad MJ, Oskoei DS, Esmaeilijah N (2018) Determine and compare the volume and length of the upper airway using cone-beam computed tomography images in patients with obstructive sleep apnea. Asian J Pharm 12(2):S484–S489
Chen H, Aarab G, Lobbezoo F, De Lange J, Van der Stelt P, Darendeliler MA, Cistulli PA, Sutherland K, Dalci O (2019) Differences in three-dimensional craniofacial anatomy between responders and non-responders to mandibular advancement splint treatment in obstructive sleep apnoea patients. Eur J Orthod 41(3):308–315. https://doi.org/10.1093/ejo/cjy085
Mostafiz WR, Carley DW, Viana MGC, Ma S, Dalci O, Darendeliler MA, Evans CA, Kusnoto B, Masoud A, Galang-Boquiren MTS (2019) Changes in sleep and airway variables in patients with obstructive sleep apnea after mandibular advancement splint treatment. Am J Orthod Dentofacial Orthop 155(4):498–508. https://doi.org/10.1016/j.ajodo.2018.05.022;10.1016/j.ortho.2019.08.005
Mouhanna-Fattal C, Papadopoulos M, Bouserhal J, Tauk A, Bassil-Nassif N, Athanasiou A (2019) Evaluation of upper airway volume and craniofacial volumetric structures in obstructive sleep apnoea adults: A descriptive CBCT study. Int Orthod 17(4):678–686. https://doi.org/10.1016/j.ortho.2019.08.005
Niskanen I, Kurimo J, Järnstedt J, Himanen SL, Helminen M, Peltomäki T (2019) Effect of maxillomandibular advancement surgery on pharyngeal airway volume and polysomnography data in obstructive sleep apnea patients. J Oral Maxillofac Surg 77(8):1695–1702. https://doi.org/10.1016/j.joms.2019.04.001
Iwasaki T, Yoon A, Guilleminault C, Yamasaki Y, Liu SY (2020) How does distraction osteogenesis maxillary expansion (DOME) reduce severity of obstructive sleep apnea? Sleep Breath 24(1):287–296. https://doi.org/10.1007/s11325-019-01948-7
Kongsong W, Waite PD, Sittitavornwong S, Schibler M, Alshahrani F (2021) The correlation of maxillomandibular advancement and airway volume change in obstructive sleep apnea using cone beam computed tomography. Int J Oral Maxillofac Surg 50(7):940–947. https://doi.org/10.1016/j.ijom.2020.11.017
Lu RJ, Tian N, Wang JZ, Zou X, Wang JJ, Zhang M, Bai CQ, Yu KT (2020) The effectiveness of adjustable oral appliance for older adult patients with obstructive sleep apnea syndrome. Ann Cardiothorac Surg 9(4):2178–2186. https://doi.org/10.21037/apm-20-1300
Alsufyani NA, Flores-Mir C, Major PW (2012) Three-dimensional segmentation of the upper airway using cone beam CT: a systematic review. Dentomaxillofac Radiol 41(4):276–284. https://doi.org/10.1259/dmfr/79433138
Singh GD (2021) Mechanisms of upper airway remodeling following surgical interventions remain elusive. Sleep 44(11):zsab201. https://doi.org/10.1093/sleep/zsab201
Alsufyani NA, Al-Saleh MA, Major PW (2013) CBCT assessment of upper airway changes and treatment outcomes of obstructive sleep apnoea: a systematic review. Sleep Breath 17(3):911–923. https://doi.org/10.1007/s11325-012-0799-7
Andrade C (2020) Mean difference, standardized mean difference (SMD), and their use in meta-analysis: as simple as it gets. J Clin Psych 81(5):20f13681. https://doi.org/10.4088/JCP.20f13681
Acknowledgements
The authors express gratitude to the Coordination for the Improvement of Higher Education Personnel (CAPES) (CAPES/PRINT Call No. 41/2017 file number 88887.465681/2019-00) and to the Brazilian National Council for Scientific and Technological Development (CNPq), which provided Dr. Fabio Costa with a PQ fellowship in Category 2.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval and consent to participate
This article does not contain any studies with human participants or animals performed by any of the authors.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gurgel, M., Junior, C., Cevidanes, L. et al. Methodological parameters for upper airway assessment by cone-beam computed tomography in adults with obstructive sleep apnea: a systematic review of the literature and meta-analysis. Sleep Breath 27, 1–30 (2023). https://doi.org/10.1007/s11325-022-02582-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-022-02582-6